Gain Broker Loyalty with Simplified Billing
Digitally Transform Employee Benefits Billing
Give brokers the ability to add unlimited plans and delight them with error-free and timely bills,
enabling them to receive commission payments faster.

Normalize Ongoing Data Flow
Reconcile enrollment with adjustments to synchronize clean employee data to use for billing, eligibility, claims, etc.
Speed Up Workflows with Accuracy
Eliminate reporting lag times by using API- powered automation to reconcile changes in data each month. This facilitates accuracy in benefit enrollment data, payroll data, and ultimately billing/payments.
Self Service Group Portal
Electronically present bills by product line to your clients as well as allowing employers to note changes. Accept remittance via an online employer-facing portal after employers log on and approve electronic payments.
Simplified Billing Services
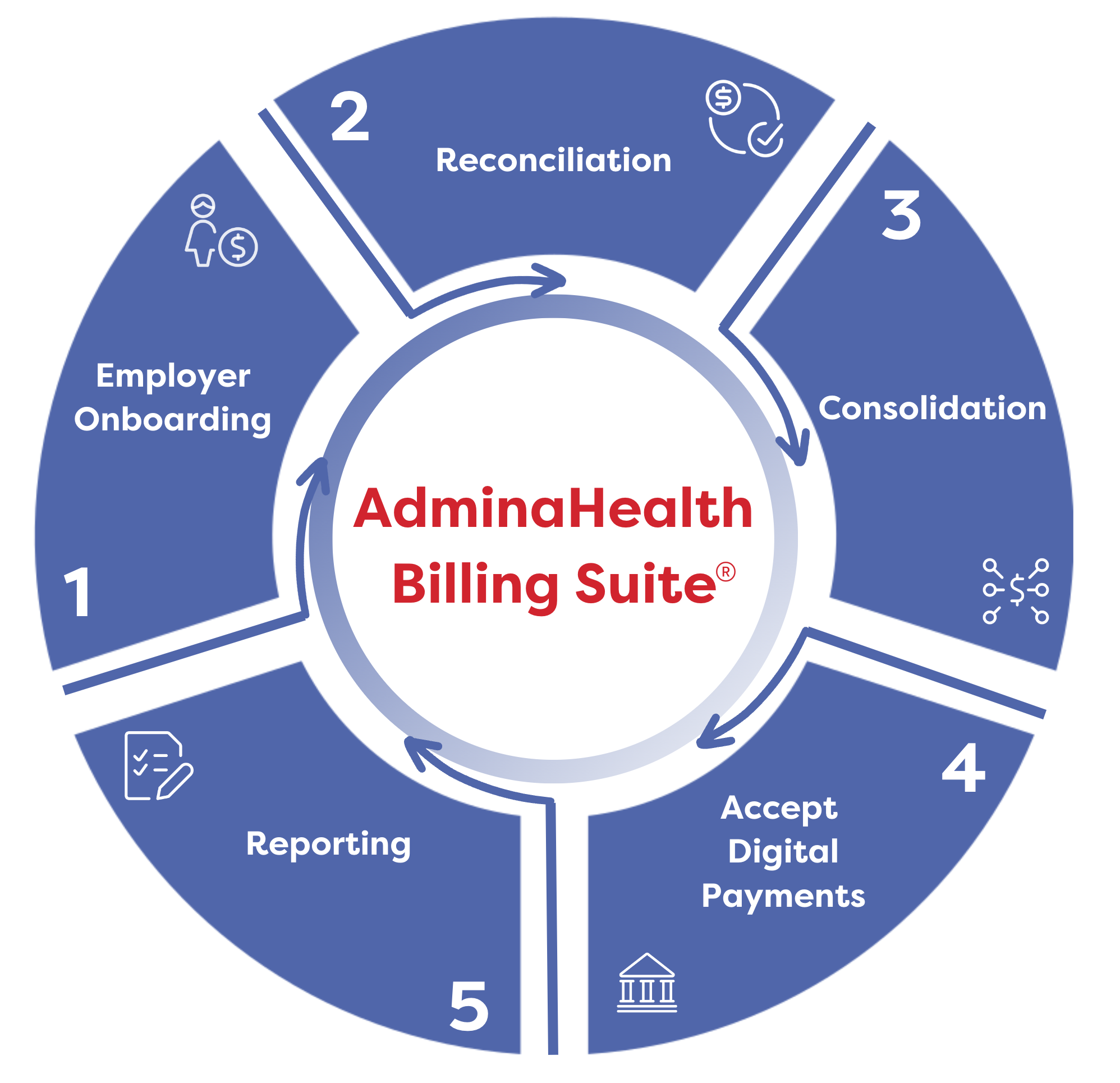
1. Employer Onboarding
Import data including Enrollments and Payroll via industry standard API, CSV, Excel, EDI, XML, or custom format. Identify and support the resolution of data integrity issues during onboarding.
2. Reconciliation
Ensure you are billing the right people the right amount through automation that uses Enrollment to verify the start of coverage the first month, and then either Enrollment or Payroll as a trigger to stop coverage each billing cycle after that. Each month the error ratio declines, giving you greater accuracy.
3. Consolidation
Post Reconciliation
Carriers can now produce a bill with a consolidated view of all product lines for digital presentment. Employers can approve and authorize a consolidated digital payment through the online portal.
Division Reporting
The consolidated view can show multiple lines of coverage by division for employer internal reporting. The invoice can be viewed online in the portal or exported and sent to each division.
4. Accept Digital Payments
Accept digital payments to your own account directly from employer accounts. Funds are transferred between employer and carrier without AdminaHealth taking fiduciary responsibility. Organizations can use their current designated bank account.
5. Reporting & Policy Admin Updates
Generate custom carrier product line reports based on your requirements such as coverage tiers, product lines, and demographics.
Data Science & Analytics
Leverage operational data over time combined with AI algorithms to drive better business decisions.
More Than a Vendor: A Trusted Partner

At AdminaHealth, we take pride in the white glove service we provide.
All partners are assigned an Implementation Manager, Data Analysts, and a Product Manager.
After onboarding, you can reach out to your Implementation Manager anytime you have questions or need help. We are here to make sure you have the support you need for your insurance benefits billing processes to run smoothly every month.

“Before implementing the AdminaHealth Billing Suite for Carriers we were struggling with managing the connections to enrollment platforms and providing accurate customer billing that included all of our product lines on a single bill. Additionally, we had no way of initiating and tracking electronic payments. Now with AdminaHealth, these problems are a thing of the past. Our brokers couldn’t be happier with the decrease in complaints and our employers are happy that they have an online portal with which to access and pay their bills.”
Trusted By












Customized Solutions

Your company has a unique workflow, ecosystem, and tech stack. The AdminaHealth Billing Suite for Carriers can provide you with customized solutions for your specific needs.
Reach out to us today for a discovery call!
[email protected]
Request a Personalized Carrier Demo

